Health
OUTCOMES
All people have the opportunity to enjoy long and healthy lives. Avoidable deaths, diseases and injuries are prevented. People have the ability to function, participate and live independently in society.
INTRODUCTION
Good health is a critical component of well-being. Good health has two core dimensions: how long people live and the quality of their lives. The health outcomes emphasise the desire to both increase length of life and reduce illness, injury and disability.
Improved health, both mental and physical, is an important aspect of reducing social exclusion. Poor health can restrict people's ability to take part fully in society, including their ability to work, to engage in and succeed at education, and to enjoy leisure and recreation activities.
A range of factors affects health outcomes, including genetic predisposition, behaviour, the environment and the availability of health services. Increasing attention is also being paid to the role of socio-economic inequalities in influencing health. There is much evidence that those with low incomes, poor housing and few qualifications have disproportionately poorer health.
The indicators selected for this report provide measures of life expectancy and prevalence of disability. Youth suicide is included as a measure of mental health that is of particular concern.
Two risk factor indicators are included: the young adolescent birth rate and prevalence of cigarette smoking. Births to young mothers have been linked in many studies with a greater risk of poor outcomes for both mother and baby in a range of areas. The links between cigarette smoking and poor health outcomes are well recognised. Many other risk factors could have been included, such as low birth weight and obesity. Future reports could include these indicators as well as others related to mental health and people's own perceptions of their health.
KEY POINTS
- Life expectancy is increasing although the rate of increase is not as great as in many other similar countries. Females continue to have a greater life expectancy than males, but this gap is narrowing as male life expectancy increases at a faster rate. Māori life expectancy is on average lower for both males and females than for non-Māori.
- The dependent disability rate shows that currently just over 11 per cent of the total population have some form of disability that requires assistance. Thirty-eight per cent of the older population have some form of dependent disability. Over the age of 75, women have slightly higher rates of dependent disability than men. Māori have higher rates of dependent disability than non-Māori at all ages, reflecting generally higher levels of chronic illness and injury.
- Independent life expectancy is an estimate of how long a person can expect to live independently, that is, free from disability requiring assistance. On average, females can expect to live around 68 years independently while for males the figure is around 65 years.
- Youth suicide rates have increased in developed countries in the last two decades and New Zealand rates are particularly high. Gender differences are marked: young males are particularly at risk of death by suicide and in 1998 accounted for three-quarters of all youth suicides. Māori are over-represented, with nearly a third of all youth suicides in 1998 being by young Māori. Females account for the majority of suicide attempts that do not result in death with non-Māori females having the highest rate.
- The young adolescent birth rate has been declining in New Zealand but is still relatively high. There are significant ethnic differences, with Māori having a higher rate of under 18 births than non-Māori, although these differences are reducing. New Zealand is currently ranked third among OECD countries for teenage birth rates.
- The prevalence of cigarette smoking among people over 15 has declined since the mid-1980s from 30 per cent to 25 per cent. Young women are still more likely to smoke than young men. Rates of smoking for Māori are twice as high as the average overall, with Māori females having the highest rates of all. Smoking rates among Pacific males are also high. Smoking prevalence is highest among those living in the most deprived areas. The prevalence of smoking by males in New Zealand is low by OECD standards while for females it is average.
SUMMARY
Three of the key indicators chosen show improvements: life expectancy, the under 18 birth rate and the prevalence of smoking. Youth suicide rates in New Zealand have remained stable for the last three years. They are, however, very high in relation to other countries. There are considerable age, gender and ethnic differences in these outcomes. Women have longer life expectancy and independent life expectancy; young males have higher rates of suicide than young women. Older people, not surprisingly, have a much higher dependent disability rate. Māori on average have lower life expectancy and independent life expectancy, and higher disability, youth suicide and young adolescent birth rates. They are also far more likely to smoke.
For many indicators, little information is available for groups other than Māori and non-Māori. Work to improve information about health outcomes for Pacific peoples and the increasingly large number of other people from other ethnic groups is continuing. Changes in definitions and classification of ethnicity for Māori and other ethnic groups also create difficulties in comparing results across time.
Where available, regional differences point to poorer health outcomes being higher in areas rated as more deprived or with higher proportions of Māori and Pacific peoples.
Life expectancy
DEFINITION
Life expectancy indicates the number of years that a person could expect to live on average, based on the mortality rates of the population in a given year.
RELEVANCE
Life expectancy at birth is a key summary indicator of population health outcomes, specifically fatal outcomes. Improvements in overall life expectancy reflect changes in social and economic conditions, lifestyle changes, medical advances and better access to health services.
CURRENT LEVEL AND TRENDS
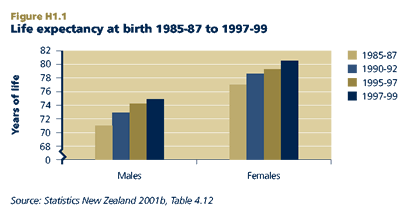
In 1997-99, life expectancy at birth was 75.2 years for males and 80.4 years for females. Since the mid-1980s, gains in longevity have been greater for males than for females. Between 1985-87 and 1997-99, life expectancy at birth increased by 4.1 years for males and 3.3 years for females.
With the decline in the infant mortality rate (from 11.2 deaths per 1,000 live births in 1986 to 5.6 per 1,000 in 1999), the impact of infant death on life expectancy has fallen.
ETHNIC DIFFERENCES
In 1995-97, the difference in Māori and non-Māori life expectancy at birth was eight years for males and nine years for females. Higher Māori mortality rates at ages 40-79 years account for most of the ethnic differences in longevity3.
Māori life expectancy at birth improved remarkably from the 1950s to the mid-1980s, increasing by 13 years for males and by 16 years for females. In the 1950s and early 1960s, almost all of the improvement in Māori life expectancy at birth resulted from reductions in infant and child mortality. In the 1970s and early 1980s, the greatest improvements in survival were at older ages.
Between 1985-87 and 1990-92, increases in life expectancy were smaller for Māori (0.5 and 0.7 years for males and females respectively) than for non-Māori (2.5 and 2.1 years). Because of a change in the ethnicity classification in 1995, the rates for 1995-97 cannot be compared with earlier years. Therefore it is not possible to say how the trend changed over the 1990s.

The life expectancy of Pacific peoples living in New Zealand is difficult to calculate because of small numbers and high levels of migration. The Ministry of Health estimates that in 1995-97, Pacific males had a life expectancy at birth of 69.8 years, and Pacific females 75.6 years.
REGIONAL DIFFERENCES
Life expectancy at birth varies by region, ranging from a high of 77.7 years in Canterbury, to a low of 73.3 years in Gisborne, a difference of 4.4 years. This difference may be related to the high proportion of Māori in the Gisborne region (45 per cent in 1996) compared with Canterbury (seven per cent).
There is a strong association between life expectancy and the level of deprivation in the area where people live. In 1995-97, males in the least deprived 10th of small areas in New Zealand could expect to live 9.2 years longer than males in the most deprived 10th of small areas (meshblocks with median populations of 90 people). For females, the difference was smaller, but still substantial, at 6.7 years. There was also a substantial difference in life expectancy for Māori males and females, according to the level of deprivation in their area (7-8 years). These figures clearly illustrate the links between socio-economic status and health.
INTERNATIONAL COMPARISON
Despite improvements in life expectancy in New Zealand over recent decades, longevity in other countries has improved faster and the levels in this country remain lower than those found in Japan, Australia, Canada and many European countries. Among OECD countries, New Zealand males are ranked somewhat higher (11th out of 28 OECD countries in 1998) than New Zealand females (17th) in life expectancy ratings.
Dependant disability
DEFINITION
The proportion of the population who acknowledge one or more functional limitations and require assistance, either intermittently or on a daily basis, to live independently.
RELEVANCE
The dependent disability rate is an important measure of non-fatal health outcomes.
CURRENT LEVEL (NO TREND DATA AVAILABLE)
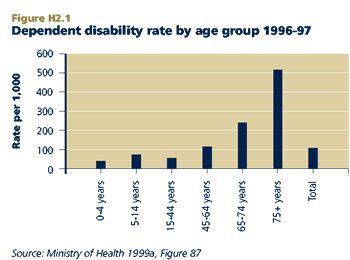
In 1996-97, 114 people per 1,000 population (or just over 11 per cent of the population) were living with disability that was classified as dependent (requiring assistance). This represents an estimated 405,000 New Zealanders.
AGE DIFFERENCES
Nearly a third (29 per cent) of those living with a dependent disability are aged 65 or over, and they comprise 38 per cent of the total older population.
Almost 15 per cent of disabled older people needing assistance (approximately 23,000, or just over five per cent of the total older population) are estimated to be living in residential care.
Twenty-seven per cent of people with dependent disability require assistance on a continuing or daily basis. This represents a rate of severe disability in the total population of 31 per 1,000 (just over three per cent).
Dependent disability increases sharply from middle age, rising from a rate of 59 per 1,000 for ages 15-44 to 550 per 1,000 for those 75 and over. Among children, levels of dependent disability are lower for those aged under five years (41 per 1,000) compared to school-aged children (79 per 1,000). Because childhood dependent disability is defined somewhat differently from that of adults, the rates for children and adults are not strictly comparable.
GENDER DIFFERENCES
Females make up a higher proportion (54 per cent) of the dependently disabled population overall, reflecting their higher dependent disability rates at the older ages and their longer life expectancy.
Among children, males are more likely to experience dependent disability than females, the risk being approximately 46 per cent higher in the 0-14 year age group. This reflects both biological and behavioural differences, including the higher risk of injury among boys.
ETHNIC DIFFERENCES
After taking into account differences in the age and gender distribution of the Māori and non-Māori populations, Māori are more likely to be dependently disabled than non-Māori (118 per 1,000 compared with 90 per 1,000). This difference is apparent in all age groups and is consistent with higher rates of chronic illness and injury experienced by Māori across most age groups

INTERNATIONAL COMPARISON
The rate of dependent disability in New Zealand appears to be higher than that reported in similar studies in Australia, Canada and the United States, although this may be influenced by differences in the collection and classification of data.
Independent life expectancy
DEFINITION
The number of years a person can expect to live independently, i.e. without any functional limitation requiring the assistance of another person or complex assistive device.
RELEVANCE
Independent life expectancy (ILE) is an integrated measure of health expectancy, capturing both "quantity" and "quality" of life dimensions of health. It is a positive measure, capturing expectations of life free from disability requiring assistance (dependence).
CURRENT LEVEL (NO TREND DATA AVAILABLE)
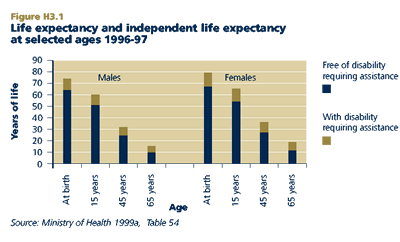
In 1996, males had an independent life expectancy at birth of 64.6 years. The figure for females was 67.9 years. These figures mean that males can expect to live independently for 87 per cent of their lives, and females for 85 per cent. Because the impact of disability greatly intensifies from middle age, the ratio of ILE to life expectancy declines sharply from around age 45. However, at age 65 almost two-thirds of remaining life expectancy will still be spent independently.
GENDER DIFFERENCES
Females spend a higher proportion of their lives needing assistance than males do. In absolute years, females can expect to live longer, both independently and in a state of dependency, than males.
ETHNIC DIFFERENCES
Māori spend more years requiring assistance than non-Māori, both in absolute years (females) and as a proportion of their shorter lives (both sexes).
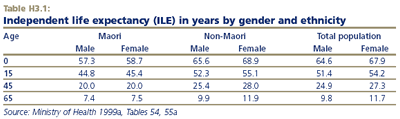
In 1996, ILE at birth for Māori males was 57.3 years, 8.3 years less than for non-Māori males. Māori females had an ILE at birth of 58.7 years, a gap of 10.2 years compared to non-Māori females.
INTERNATIONAL COMPARISONS
In June 2000, the World Health Organisation (WHO) reported on a new health expectancy measure. Whereas the ILE is based on a single dependency threshold - disability requiring assistance - in the Disability Adjusted Life Expectancy (DALE), the years of disability are weighted according to severity and subtracted from the expected overall life expectancy to give the equivalent years of healthy life. There is currently no robust information for New Zealand but the Ministry of Health intends to replace the ILE measure with DALE when this becomes available.
Youth suicide
DEFINITION
The number of suicide deaths of persons aged 15-24 as a proportion (per 100,000) of the population in that age group.
RELEVANCE
Suicide at any age is a concern but rising rates of youth suicide in a number of countries over the past 20 years have made youth suicide an issue of international attention. Changes in the rate of youth suicide may reflect the level of support available to young people as they make the transition to adulthood. Suicide is the second leading cause of death (after motor vehicle deaths) for New Zealand young people aged 15-24 years.
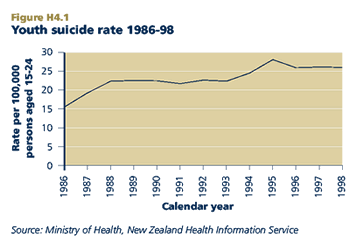
CURRENT LEVEL AND TRENDS
In 1998, there were 140 deaths from suicide among young people aged 15-24, a rate of 26.1 per 100,000 in that age group. The youth suicide rate in 1998 was 67 per cent higher than the rate in 1986 (15.6 per 100,000), having risen sharply in the late 1980s and again in the mid-1990s. The youth suicide rate has remained unchanged over the last three years.
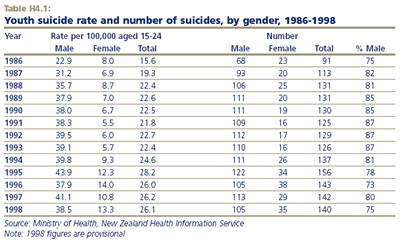
GENDER DIFFERENCES
Males have a much higher rate of youth suicide than females, with 38.5 suicides per 100,000 compared to 13.3 per 100,000 in 1998. Males accounted for the sharp rise in youth suicide in the late 1980s, whereas females accounted for most of the rise in the mid-1990s.
While males account for most youth suicide deaths (75 per cent in 1998), females account for the majority of recorded suicide attempts that do not result in death (65 per cent in 1999). In 1999, 1,073 persons aged 15-24 were admitted to hospital with self-inflicted injuries. In contrast to the youth suicide death rate, females (266.7 per 100,000) were more likely than males (139.9 per 100,000) to be admitted to hospital for this reason.
ETHNIC DIFFERENCES
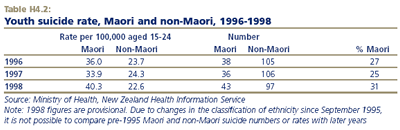
In 1998, 43 Māori youth aged 15-24 years died from suicide. Māori youth appear to be over-represented among 15-24 year olds who die from suicide, accounting for 31 percent of all youth suicides in 1998, but only 20 percent of 15-24 year olds.
Youth suicide rates for Māori are subject to considerable annual fluctuation because of small numbers and trends over time are therefore difficult to interpret. However, the rate of suicide among young Māori appears to be consistently higher than for non-Māori.
In 1998, the youth suicide rate for Māori was 40.3 per 100,000 compared to 22.6 for non-Māori. Rates of hospitalisation for attempted suicide are highest among non-Māori females (280.6 per 100,000 in 1999), followed by Māori females (213.2), Māori males (166.0) and non-Māori males (133.4).
INTERNATIONAL COMPARISONS
A comparison of youth suicide rates in selected OECD countries shows that New Zealand has the highest rate of suicide among 15-24 year olds, followed by Finland, Australia and Norway.
Birth to young adolescents
DEFINITION
The number of live births to females aged less than 18 years of age as a proportion (per 1,000) of the number of females aged 13-17 years.
RELEVANCE
Childbearing among young adolescents has been associated with a number of negative outcomes for both mother and child including low child birth weight, increased risk of infant mortality, reduced maternal educational attainment, reduced participation in paid work, and increased risk of long-term reliance on income support.
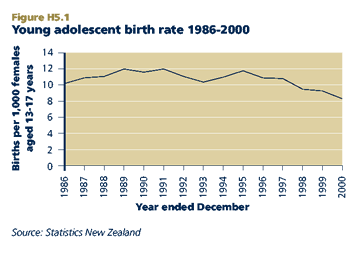
CURRENT LEVEL AND TRENDS
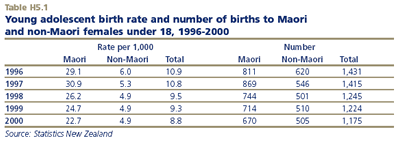
In 2000, there were 1,175 births to females under 18, representing a rate of 8.8 births per 1,000 females aged 13-17. The under-18 birth rate rose in the late 1980s, fluctuated between 10-12 per 1,000 in the early 1990s and has declined since 1995 to below the level in the mid-1980s.
Births to females under 18 accounted for two per cent of all births in 2000. The vast majority of these (97%) were to 15-17 year olds.
ETHNIC DIFFERENCES
The rate of childbearing among young Māori under 18 is significantly higher than the non-Māori rate. In 2000, there were 22.7 births per 1,000 to Māori females compared to 4.9 for non-Māori. Of the 1,175 under-18 births in 2000, over half (670) were to Māori. Births to young Māori under 18 accounted for five per cent of all births to Māori women in 2000.
Since 1996 there has been a sharp decline in the Māori under-18 birth rate from 29.1 per 1,000 to 22.7 in 2000. As a result, the ethnic difference in the rate of adolescent childbearing has narrowed.
Rates of childbearing among young Pacific females are produced by Statistics New Zealand for Census years only. In 1996, the birth rate for Pacific females aged 13-17 was 17.0 per 1,000.
REGIONAL DIFFERENCES
During 1995-97, Gisborne (20.2), the Bay of Plenty (17.0) and Northland (15.6) had the highest rates of births to women under 18. Tasman (3.4) and Otago (5.8) had birth rates below the New Zealand average of 8.8 per 1,000. Regional differences may reflect differences in the ethnic composition of the area; variations in employment and economic opportunities across regions; and differences in the level of access to birth control services.
INTERNATIONAL COMPARISONS
Data on birth rates for young women under 18 is not readily available for many countries. The under-20 birth rate is used for comparison instead.
New Zealand has relatively high teenage birth rates compared with other developed nations and for most of the past decade was second only to the United States on this measure.
With a rate of 29.5 births per 1,000 women aged 15-19 in 1999, New Zealand is now in third place behind the United States (51.1 per 1,000), England and Wales (30.9 in 1998) and Scotland (30.9 in 1997). This compares to very low rates of teenage childbearing in the Scandinavian countries and the Netherlands. Over the 1990s, teenage childbearing rates declined in many developed countries, including New Zealand and the United States.
Prevalence of cigarette smoking
DEFINITION
The proportion of the population aged 15 and over who smoke cigarettes, as measured in consumer surveys conducted by ACNielsen.
RELEVANCE
Tobacco smoking is a well-recognised risk factor for many cancers and respiratory and cardiovascular diseases. In addition, exposure to environmental tobacco smoke (particularly maternal smoking) has been identified as a major risk factor for Sudden Infant Death Syndrome (SIDS) and respiratory problems in children. Internationally, smoking has been identified as the major cause of preventable death in OECD countries.
CURRENT LEVEL AND TRENDS
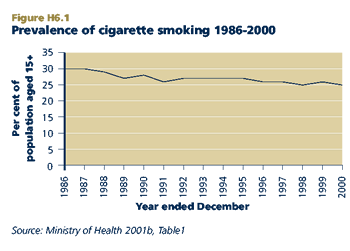
In 2000, 25 per cent of New Zealanders aged 15 years and over were cigarette smokers. The prevalence of smoking has declined from 30 per cent in 1986, with most of the decline occurring between 1987 and 1991.
AGE AND GENDER DIFFERENCES
Smoking is most prevalent among people aged 25-34 years, followed by those aged 15-24 and people aged 35-54. Older people aged 55 and over are much less likely to smoke and have experienced the greatest decline in smoking prevalence over the past 15 years. Whereas in 1986 women were slightly more likely to smoke than men (31 and 29 per cent respectively), smoking prevalence was the same for both sexes in 2000 (25 per cent).
However, among 15-24 year olds, females are still more likely to smoke than males. There is little difference in smoking prevalence between males and females aged 25-34, but for those aged 35 and over smoking has generally been more prevalent among males, with both genders becoming less likely to smoke over the 1990s.
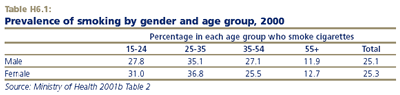
ETHNIC DIFFERENCES
Māori women have the highest smoking prevalence (52.5 per cent), followed by Māori men (45.3 per cent). Smoking prevalence among Māori has remained relatively unchanged over the 1990s.
Among Pacific peoples, smoking is much more prevalent among men (40.5 per cent), than among women (28.5 per cent).

REGIONAL DIFFERENCES
The proportion of smokers is related to the level of deprivation in an area. An analysis of 1996 Census data shows a two-fold to three-fold increase in the proportion of smokers in the most deprived (decile 10) areas compared to the least deprived (decile 1) areas for all age groups, for both men and women.
INTERNATIONAL COMPARISON
In the late 1990s New Zealand males had the second lowest smoking prevalence rate of 28 OECD countries (after Sweden, 17 per cent) while females were ranked 13th. New Zealand is among those countries with little gender difference in smoking rates. In some of the countries with lower female rates than New Zealand, there is a large gender difference in smoking prevalence. For example in Japan, 53 per cent of men smoked compared with 13 per cent of women.
